

With extensive training, experience, and dedication to patient care offering the comprehensive services tailored to meet the unique needs of each individual.

Our body has some different types of cells that behave like nerve cells in certain ways and like hormone-making endocrine cells in other ways. These cells do not form an actual organ, instead, they are scattered throughout other organs like the oesophagus, stomach, pancreas, intestines, and lungs.

Like most cells in the body, GI tract neuroendocrine cells sometimes go through certain changes that cause them to grow too much and form tumors. These tumors are known as neuroendocrine tumors (NET) and neuroendocrine cancers. In the past, most abnormal growths of neuroendocrine cells were called carcinoids.
But in 2000, the World Health Organization (WHO) reclassified carcinoids into neuroendocrine tumors and neuroendocrine cancers.
Neuroendocrine tumors are growths that look benign (i.e not cancerous) but that might possibly be able to spread to other parts of the body. Neuroendocrine cancers are abnormal growths of neuroendocrine cells which can spread to other parts of the body.
Neuroendocrine cancers (also known as neuroendocrine carcinomas) can then be divided into groups based on the way the cells look under the microscope. A cancer with cells that do not look very abnormal is called well differentiated. These tumors tend to be less aggressive. They grow and spread slowly. Well differentiated neuroendocrine cancers can look identical to benign neuroendocrine tumors when examined under the microscope.
Sometimes the only way to know for certain that a mass is a neuroendocrine cancer (and not a benign tumor) is when it spreads to other organs or tissues. If the cells of a cancer look very abnormal, it is called poorly differentiated. These cancers tend to be more aggressive meaning that they grow and spread quickly.
In general, neuroendocrine tumors and neuroendocrine cancers grow more slowly than other cancers in the GI tract. But how they grow and whether or not they spread to other areas varies widely. This depends to some extent on which part of the body the tumor starts in.

A risk factor is anything that affects your chance of getting a disease such as cancer. For example, exposure to strong sunlight is a risk factor for skin cancer, while smoking is a risk factor for cancer of the lung, and several other cancers. But risk factors don’t tell us everything. Someone without any known risk factors can still develop cancer. And someone can have a risk factor, but still not get the disease.
Risk factors, however, do not reveal everything. A person’s likelihood of contracting the disease is not necessarily determined by the presence of one or more risk factors. Additionally, many individuals who contract the disease may not have any known risk factors.


Most tumors grow slowly and produce vague symptoms that are more often caused by something else. When trying to figure out what’s going on, doctors and patients are likely to explore other, more common possible causes first. This can delay a diagnosis, sometimes even for several years.
People with tumors/cancers in their appendix often don’t have symptoms. If it is discovered, it is often when they have their appendix removed during an operation for some other problem.
The symptom a person develops from a gastrointestinal neuroendocrine tumor often depends on where it is located. Pancreatic neuroendocrine tumors are most often non-functional and are often detected incidentally. Functional tumors produce hormones and are responsible for symptoms for eg Insulinoma produces insulin and lowers blood sugar levels, Gastrinoma produces gastrin and causes hyperacidity, VIPoma produces a peptite that is reposnsible for severe and oft repeated diarrhoea.

Carcinoid tumors that develop in the stomach usually grow slowly and often do not cause symptoms. They are sometimes found during an exam of the stomach by endoscopy that is done to look for other things. Some can cause symptoms such as the carcinoid syndrome.

Facial flushing involves sudden redness and warmth in the face, which can occur due to hormonal changes caused by neuroendocrine tumors.

Severe diarrhea is a common symptom of neuroendocrine tumors (NETs), caused by the overproduction of hormones like serotonin and gastrin. This excessive hormone secretion disrupts normal gastrointestinal function.

Symptoms may include wheezing, rapid heartbeat, and palpitations, which can occur due to excess hormone production by neuroendocrine tumors, affecting heart and lung function.

General approach to this kind of treatment is different approach. The main factors in selecting treatment options for a neuroendocrine tumor are:
This section lists common tests that may be performed and it is not necessary for all the tests to be performed for a patient. Your doctor will select the tests that will assist him /her to have the maximum information about the tumor/ disease.
Other commonly used tests to look for carcinoids can include blood tests for chromogranin A (CgA), and gastrin. Depending on the where the tumor might be located and on the patient’s symptoms, doctors may do other blood tests as well. Some of these tests can also be used to show how well treatment is working, since the levels of these substances tend to go down as tumors shrink.
Tests of the blood and urine can be very helpful in diagnosing carcinoid syndrome in patients who have symptoms that may be caused by it.
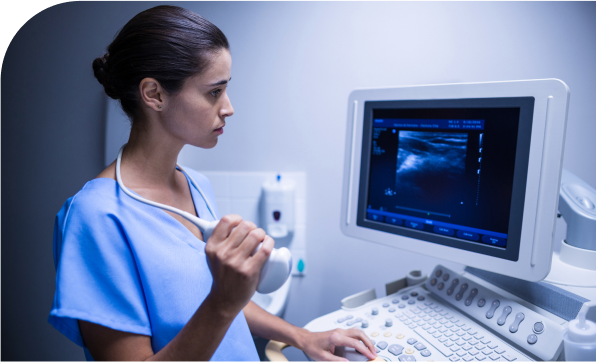
his test uses an endoscope with a small ultrasound probe on the end. This probe releases sound waves and then detects the echoes that bounce off tissues of the digestive tract wall. A computer then translates the pattern of echoes into an image of the wall of the esophagus, stomach, intestine, or rectum.
Putting the ultrasound probe on the end of an endoscope lets it get very close to the tumor. Because the probe is close to the area being studied, it can make very detailed pictures. EUS can be used to see how deeply a tumor may have grown into the wall of the esophagus, stomach, intestine, or rectum.
Endoscopic ultrasound can also help see if certain lymph nodes are enlarged and help a doctor guide a needle into a lymph node, tumor, or other suspicious area to do a biopsy.
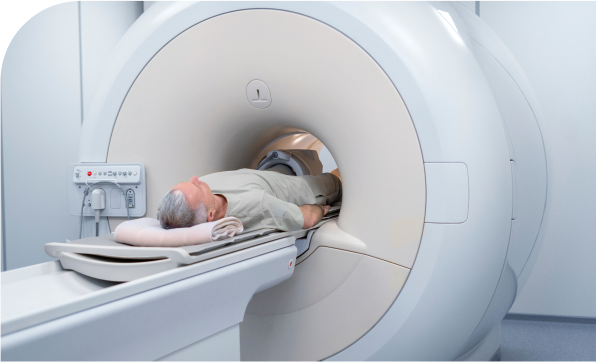
A CT scan is a type of x-ray that gives a picture of organs and other structures (including any tumours) in your body. It is used to see more details of a cancer and its relation to the surrounding organs in your body. It also gives information related to cancer spread into the lymph nodes, liver or lungs.
CT scans can help tell if your cancer has spread into lymph nodes or other organs such as your liver. They can also be used to guide a biopsy needle precisely into a suspected area of cancer spread. For a CT-guided needle biopsy, the patient remains on the CT scanning table, while a doctor moves a biopsy needle in the body toward the location of the mass.
CT scans are repeated until the doctor is sure that the needle is in the mass. A fine-needle biopsy sample (tiny fragment of tissue) or a core-needle biopsy sample (a thin cylinder of tissue about ½-inch long and less than 1/8-inch in diameter) is then removed and looked at under a microscope.
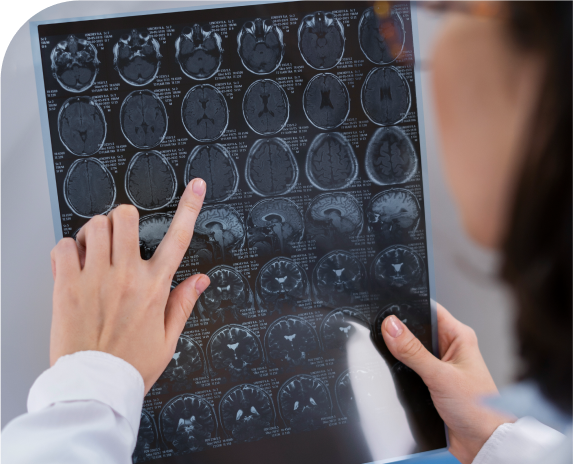
Scans using small amounts of radioactivity and special cameras may be helpful in looking for neuroendocrine tumors. They can help determine the extent of the tumor, as well as help locate it if doctors aren’t sure where it is in the body.

A positron emission tomography (PET) scan is another imaging test that uses low levels of radioactivity to look for tumors. For most diseases, PET scans use a form of radiolabelled glucose (sugar) to find tumors. But when it is used to look for neuroendocrine tumors/cancers, PET uses a radioactive form of 5-hydroxytryptophan (5-HTP), a chemical that is taken up and used by neuroendocrine cells.
A special camera can detect the radioactivity. Some doctors have found PET scans to be more accurate than CT scans for detecting spread of disease. However, this technique is not available in every hospital.

Even if an imaging test finds a mass, it cannot tell if the mass is a neuroendocrine tumor, some other type of tumor or cancer, or an area of infection. The only way to know for sure is to remove cells from the abnormal area and look at them under a microscope. This procedure is called a biopsy.
There are several ways to take a sample from a gastrointestinal tumor. One way is through the endoscope. When a tumor is found, the doctor can use a biopsy forceps (pincers or tongs) through the tube to take a small sample of it. Another way to sample a tumor is with a CT-guided needle biopsy, as was described in the section on CT scans.

This test is like a CT scan, but it uses magnetism instead of x-rays to build up pictures of the organs in your abdomen. Like a CT scan, MRI is painless and the magnetism is harmless. MRI scan may be used to see the extent of blockage of bile duct and in case the patient is allergic to contrast dye injection used for CT scans.

Somatostatin receptor scintigraphy, also known as OctreoScan, is the scan most commonly used to look for neuroendocrine tumors. It uses a hormone-like substance called octreotide that has been bound to radioactive indium-111. Octreotide attaches to proteins on the neuroendcorine cells.
A small amount of this substance is injected into a vein. It travels through the blood and is attracted to neuroendocrine tumor cells. About 4 hours after the injection, a special camera is used to show where the radioactivity has collected in the body. More scans may be done over the next few days as well.

Surgery remains the best option of treatment for Neuroendocrine tumors. Unlike other cancers these tumors tend to grow slowly but occasional tumors can be aggressive as well. Unlike other organ cancers if tumor shows signs of spread (metastases), it can still be treated aggressively by removal or destruction of the tumors. Example a surgeon may not give too much hope for a person with Stomach Cancer that has spread to the liver but a person with neuroendocrine tumor that has spread to the liver will still be treated aggressively and may even get cured.
Several types of operations may be used to treat neuroendocrine tumors. Some of these remove the primary tumor (where the cancer started), while others remove or destroy cancer spread (metastases) in other organs such as RFA (radiofrequency ablation).

Chemotherapy uses anti-cancer drugs that are injected into a vein or a muscle or taken by mouth to kill cancer cells. These drugs enter the bloodstream and reach all areas of the body, making this treatment useful for some types of cancers that have spread to other organs.
Unfortunately, not many neuroendocrine tumors respond to chemotherapy. Because of this, chemotherapy generally is used only for tumors that have spread to other organs, are causing severe symptoms, and have not responded to other medicines. Tumors may be treated with more than one drug, although it’s not clear that this is any more effective than using a single drug. New chemotherapy drugs and combinations of drugs are being studied.
Interferon-alfa is sometimes helpful in shrinking or slowing the growth of metastatic neuroendocrine cancers and improving symptoms of carcinoid syndrome.
Normally, chemotherapy drugs enter the bloodstream and can travel throughout the body. When carcinoid cancer has spread to the liver, it is sometimes treated by directly injecting the chemotherapy drug into the hepatic artery, which supplies blood to parts of the liver.
This exposes the liver tumors to high doses of the drug but limits exposing the rest of the body. Sometimes the chemotherapy drug is injected together with a material that plugs up the artery (an approach called chemoembolization). When the arteries leading to them are blocked, the tumors become starved for nutrients and oxygen and many die off.
Several newer types of drugs, known as targeted therapies, are now being studied for use against neuroendocrine tumors and cancers. These drugs are designed to attack some specific aspect of cancer cells. Bevacizumab (Avastin®), for example, attacks a tumor’s blood supply. It is already being used against some types of cancer and is being studied for these tumors. Other targeted therapies block the molecules that increase the growth of cancer cells. Some of these (such as erlotinib, temsirolimus, sorafenib) are used in other types of cancer and are now being tested against carcinoids.
Radionuclide scans
,such as the Octreoscan, can be helpful in finding neuroendocrine cancers because they use substances that are attracted to neuroendocrine cells.

Dr. Deepak Chhabra is a consultant Surgical Oncologist with an extensive experience in cancer surgeries. He is has specialized in Hepato (Liver) -Biliary (Gallbladder) and Pancreatic Cancer Surgeries.

Take the first step towards your journey to wellness by scheduling an appointment with Dr. Deepak Chhabra, a trusted oncologist dedicated to providing compassionate care and personalized treatment plans.
Discover first hand accounts from patients who have experienced compassionate care and expert treatment at our clinic. Read their reviews to get to know their journey.
5 Out of 5 from 92 Reviews
